Pereira-Céspedes A, Hernández Soto LE, Lizano-Barrantes C
Universidad de Costa Rica. Facultad de Farmacia. Instituto de Investigaciones Farmacéuticas. San José (Costa Rica)
Fecha de recepción: 02/05/2020 – Fecha de aceptación: 10/06/2020
Correspondencia: Alfonso Pereira Céspedes – Cuidad Universitaria Rodrigo Facio – Universidad de Costa Rica, Facultad de Farmacia, INIFAR – 11501 San José (Costa Rica)
alfonso.pereiracespedes@ucr.ac.cr
____
SUMMARY
Introduction: Minor Ailment Service is a very common pharmaceutical service. The objective was to evaluate the criteria associated with the referral to physician or with dispensing medicines in those consultations in Costa Rica.
Method: Observational descriptive cross-sectional multicenter exploratory study of: Minor Ailment Service consultations in 30 community pharmacies, and analyzed the factors associated with to refer to the physician or dispense medicines.
Results: There were 1,538 consultations, of which medicines are dispensed in 92.3% of them (n=1,420), referred to the physician in 6.7% (n=103). In relation to the intervention of referring to the physician, the bivariate analysis showed a statistically significant association with them, highlighting the criteria suspected adverse drug reaction, medicines use currently for other health problem and duration of the health problem ≥7 days.
Conclusions: The service is complex and shows that the pharmacist follows a series of criteria to make a decision –the referral to physician or dispensing medicines–. There are seven important criteria according to this study. However, the one that stands out is suspected adverse drug reaction, followed by medicines use currently for other health problems, duration of the health problem ≥7 days and pregnancy/lactation.
Key words: Minor Ailments Service, community pharmacy services, pharmacist, physicians.
Servicio de Indicación Farmacéutica en Costa Rica: criterios asociados con dispensar un medicamento o derivar al médico
RESUMEN
Introducción: La indicación farmacéutica es un servicio farmacéutico muy común. El objetivo fue evaluar criterios asociados con derivar al médico o dispensar.
Método: Estudio exploratorio multicéntrico, descriptivo de las consultas de indicación farmacéutica en 30 farmacias comunitarias durante 8 semanas.
Resultados: Hubo 1.538 consultas, de las cuales se dispensaron medicamentos en el 92,3% de ellas (n=1.420), remitidas al médico en el 6,7% (n=103). En relación con la intervención de referirse al médico, el análisis bivariado mostró una asociación estadísticamente significativa con ellos, destacando los criterios sospecha de reacción adversa a medicamentos, uso de medicamentos actualmente para otro problema de salud y duración del problema de salud ≥7 días.
Conclusiones: El servicio es complejo y muestra que el farmacéutico sigue una serie de criterios para la derivación al médico o la dispensación. Hay siete criterios importantes según este estudio. Sin embargo, el que destaca es la sospecha de reacción adversa a medicamentos, seguido del uso de medicamentos actualmente para otros problemas de salud, la duración del problema de salud ≥7 días y el embarazo/lactancia.
Palabras clave: Servicio de Indicación Farmacéutica, servicios farmacéuticos, farmacéutico, médicos.
____
INTRODUCTION
There are health problems (HP) that involve a complex management and require the intervention of different professionals to evaluate it. This complexity can be given by the variety of causes of this problem, but it can also be due to the diversity of alternatives for its manageament. Although there are HP considered as minor ailments, they may have different causes and management, as mentioned above.
Minor ailments (MA) refers to self-limiting or short-lasting non-serious health problems that are unrelated to the clinical manifestations of the other health problems affecting the patient, or to the desired or undesired effects of the medicines he/she is taking. As such, they do not require a medical diagnosis1-3 and respond to or can be alleviated by a symptomatic treatment. It also refers to those health problems for which pharmacists are authorized1.
Patients experience these MA and attend to different healthcare professionals as part of their self-care2,4-6. They can go directly to their primary care physician or, often in Costa Rica, to the community pharmacy (CP) pharmacist. This is where the Minor Ailments Service (MAS) takes place, defined as “the professional service provided upon patient request in the pharmacy, when unsure of which medicinal product to acquire and upon requesting that the pharmacist provide the most appropriate remedy for a specific health problem”7.
In Costa Rican context8-10, the MAS has traditionally been offered in private community pharmacies. The pharmacist can advise without dispensing, dispense medicines, make hygienic-dietary recommendations, or refer to the physician or to the Pharmacotherapy Follow-up service, taking into account all the information gathered during the interview with the patient as part of the service8.
Pharmacists dispense both over-the-counter (OTC) and some prescription medicines (for example, NSAIDs, antacids, antihistamine medicines)8. However, it is important to mention that there is no regulation for this service and there is no remuneration for the consultation. The only remuneration is the cost of the dispense medicines.
Referral to the physician depends on the evaluation and verification of some criteria established in the literature6,7,9,11.The document Classification of Pharmaco-Therapeutic Referrals states that “the implementation of pharmaceutical care procedures (…) has led to the detection of pharmacotherapy related situations which cannot be resolved by pharmacists as such situations are not within their scope of competence. This means that the patient has to be referred to another healthcare professional in order to receive effective care”12. This referral sometimes tends to be oriented to the type of health professional the patient should consult13, for example a nutritionist, a specialist physician, among others. However there are more reasons for the referral such as referral criteria used, evaluation made by the health professional, health professional training, etc.
There are criteria that pharmacists take into account to consider that the resolution of a HP exceeds its professional competences and we are trying to ascertain in this study. Some of them are included in the definition of minor ailment, others have to do with the patient: children under the age of 2, pregnancy or lactation, other HP or medicines; and others have to do with the HP in question: others medicines taken previously, suspected adverse drug reaction (ADR) or allergy, and duration6,7,14. On the other hand, some determinants of health influence the MAS, for example: country epidemiological profile, healthcare system, social status, workplaces, gender (men and women suffer from different types of diseases from at different ages)15.
Referring to the physician, in general, reflects a commitment to the quality of care provided and is evidence that “in order to provide appropriate healthcare, therefore, the pharmacist’s referral to a doctor (and vice versa) is a professional need and obligation”16. However, “the decision of whether a patient should be referred or not to the physician is not easy and should prevail the principle primum non nocere”16.
The aim of this study was to evaluate the criteria associated with the referral to physician or with dispensing medicines in the Minor Ailment Service (MAS) consultations in Costa Rica, in order to start describing this service.
Material and Methods
This was an observational, descriptive cross-sectional multicenter exploratory study in 30 community pharmacies in Costa Rica metropolitan area. No restrictions to participant community pharmacies were applied. Community pharmacists received additional training about the study protocol and instruments.
MA consultations that took place during eight consecutive weeks in 2014 were characterized. The Inclusion criterion was any patient, caregiver or other older than 18 years that consulted for a MA, excluding the ones that could not communicate in spanish. All kinds of MA according to community pharmacist expertise were considered.
Data collection was obtained from the evaluation of consultations notes self-reported by pharmacists. Then nine criteria (variables) defined by MAS guidelines were studied, evaluating the influence of each of them (independent variable) on the referral to the physician or on the dispensing of medicines (dependent variables).
These criteria were: under the age of 2, other HP, medicines used currently for other HP, medicines taken previously for the HP in question, pregnancy or lactation, suspected ADR, drug allergies, food allergies and duration of the HP ≥7 days.
As part of the statistical analysis, using SPSS v19, the association measure (odds ratio) of each independent variable and each dependent variable (univariate analysis) was estimated, considering a statistical significance of p<0.05. The study complied with the current bioethics regulations in Costa Rica, including Helsinki declaration, and ethical permission was obtained by University of Costa Rica Ethics Committee. More details are described elsewhere8.
RESULTS
There were 1,538 MA consultations, of which medicines were dispensed in 92.3% of them (n=1,420), referral to the physician in 6.7% (n=103) and other interventions were carried out in the remaining 1,0%.
Of the 1,420 consultations where medicines were dispensed, in 16.9% (n=240) patients were also referred to the physician if the HP did not improve. On the other hand, regarding to referral to the physician, 78.6% (n=81) were referred without any other intervention, while 21.3% (n=22) were given hygienic-dietary recommendations, as well.
The three main types of consultations were related to respiratory system diseases (flu, cough and cold) (27,8%, n=427), digestive system diseases (diarrhea, irritable bowel syndrome and toothache) (16,8%, n=258) and musculoskeletal system and connective tissue diseases (muscle contracture and limbs pains) (11,3%, n=174). The other 44,1% of the minor ailments were mainly related to skin (urticaria, dermatitis), genitourinary (vaginitis, cystitis and dysmenorrhea) and nervous system problems (migraine, headache, acute pain). The main dispensed medicines were anti-inflammatories, antitussives, antihistamines, antacids, antispasmodics, prokinetics and anti-emetics. It should be noted that in 92% of consultations, prescription or restricted sale medicines –according to national legislation– were dispensed.
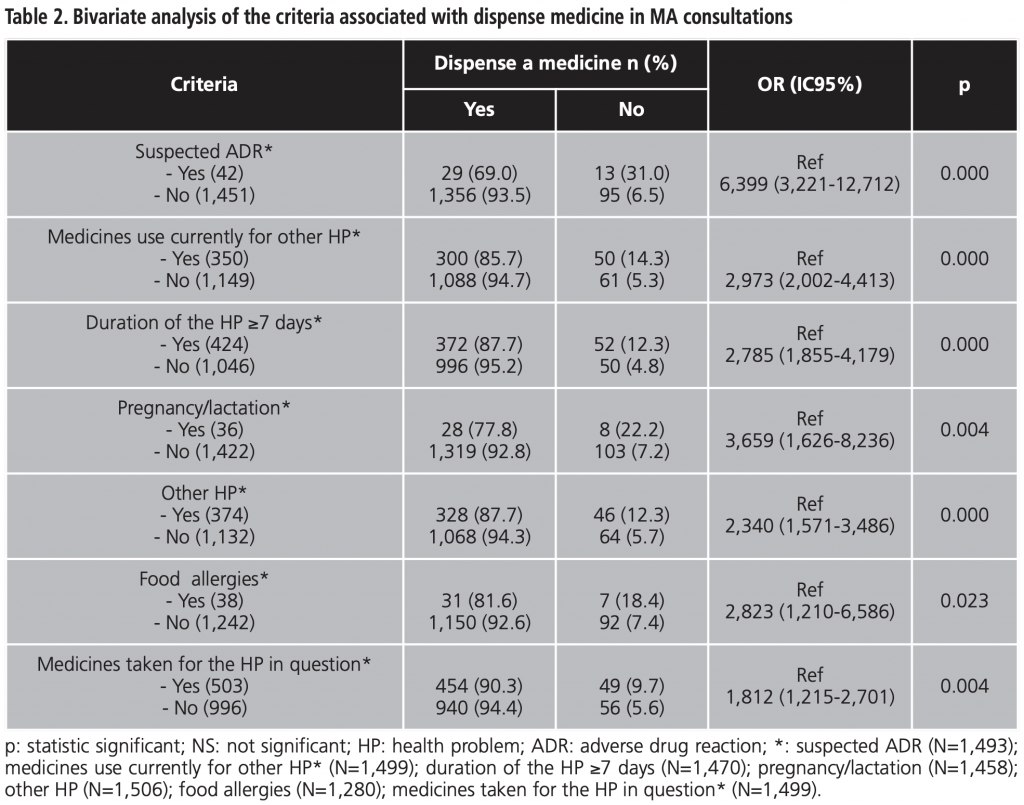
Table 1 and table 2 summarizes the seven criteria that had a statistically significant association in relation to refer to the physician or dispense medicine. The criteria under the age of 2 year did not have a statistically significant association. The criteria food allergies and drug allergies did not have a statistically significant association in relation to refer to the physician or dispense medicine, respectively
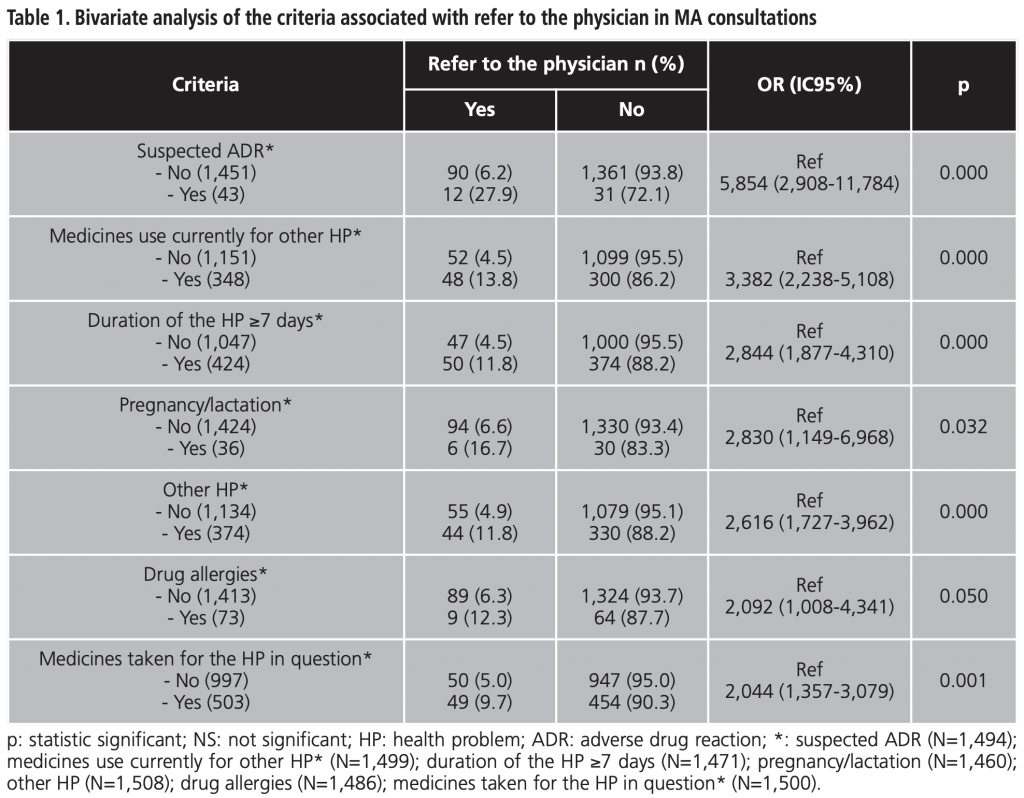
In relation to the intervention of referring to the physician, the bivariate analysis showed a statistically significant association with them, highlighting the criteria suspected ADR, medicines use currently for other HP and duration of the HP ≥7 days.
On the other hand, in relation to the intervention of dispensing medicine, the bivariate analysis showed a statistically significant association with the non-compliance of the following criteria: medicines taken for the HP in question, medicines use currently for other HP, pregnancy/lactation, suspected ADR, duration of the HP ≥7 days and other HP.
The criteria suspected ADR, duration of the HP ≥7days and pregnancy/lactation was significantly associated both with refer to the physician and dispense medicine (OR=5,8 and OR=6,3 respectively).
DISCUSSION
Pharmacists resolve consultations that end up in actions such as dispensing medicines or referral to other services in the daily work of the community pharmacy. In this scenario, the pharmacist must always evaluate certain information about the patient, its health status, its medications, the characteristics and the severity of its symptoms, the effect and the risk of dispensing medicines6,7,14,16-19.
This study aimed to evaluate, for the first time in Costa Rica, criteria associated with dispense medicines or with referral to the physician as part of the MAS. The country does not have official guidelines or protocols related to this service. However, community pharmacists, could be basing their actions on contents acquired during their Pharm D courses, continuing education programs, postgraduate programs or self-taught, aspects out of the objective of this study.
Many authors mentioned that MAS was a basic pharmaceutical service and its characteristics changed according to each country20-25. Many countries such as Australia, Canada, England, New Zealand and Spain have protocolos already established for MAS and its impact has been documented23-25.
In Costa Rica, it is a common and basic service of almost every private community pharmacy8,10, but have not protocolos already established and many factors and determinants of health influence it, such as:
The pharmacist: in Costa Rica each community pharmacy must have at least one pharmacist and this service is offered by them, different from other latinamerican countries. Community pharmacists are considered competent, accessible2,5,13,22,26 and trustful healthcare professionals2,13,22,26, which facilitates the pharmacist-patient relationship. These professionals have other tasks like: obtain, store, secure and distribute medicines and other pharmaceutical care activities. Pharmacists are responsible for all their actions in their pharmacy practice at the community pharmacy.
The patient: some of the patients’ characteristics that the community pharmacists have to consider are: age, pregnancy or lactation, other health problems, medicines used currently for other health problems4,26. In addition, they should consider cultural diversity, health literacy, the use of information and communication technologies among others5. Patients do not always proactively provide all of the information before, thus pharmacists’ communication skills become more important5,27. In most cases patients go to the community pharmacy searching for a quick solution for their consultation, thinking it is a minor ailment and asking for medication. This fact may influence pharmacists’ decision3,5,7,22,28, and it is an opportunity for responsible self-medication4,5,29.
The characteristics of the consultation: Its context, severity and urgency5 are aspects to consider.
Medicines: in Costa Rica, the arsenal of accessible medicines is extensive8 and their legislation classifies them in two categories: over-the-counter (OTC) and sale restricted (ethical or prescription). The Ministry of Health of the country focuses their control mechanisms in certain groups of medicines, such as psychotropic and narcotics. The control of the rest of medicines in community pharmacies remains mainly on the pharmacist. All the above increases the pharmacotherapeutic options that pharmacists have for the MAS5.
Costa Rica ́s epidemiological profile: cardiovascular and oncological diseases are the most predominant HP30,31. There is a probability that patients with these diseases ask the pharmacist to dispense medications for a minor health condition. According to the MAS guidelines the community pharmacist must refer to the physician in the instances of cardiovascular or oncological diseases, but it is a great opportunity to identify patients at risk and that requires a referral to other health care levels.
Costa Rica’́s healthcare system: it has a public and private sector. The public sector is led by the Caja Costarricense de Seguro Social (CCSS), an autonomous institution in charge of financing, purchasing and delivering most of the personal healthcare services in a universal manner. The private sector includes a group of ambulatory (e.g. community pharmacies) and hospital services for lucrative purposes31. Public services have a high coverage and a big demand that saturates them. On the other hand, private sector services must be paid directly by the patient and they are often inaccessible to a part of the population for their high cost31. This makes the population demand the MAS, which is free of charge, having to pay only the cost of the dispensed medicine, in case it is required. MAS implies a saving to the system2-5,20,28 for two reasons. First, a saving to the patient who invests only in the cost of the dispense medicine. Second, to the social security because the patient, instead of going to the Emergency Department or to the physician, can consult in a community pharmacy in some cases.
This study allows to analyze some criteria that community pharmacists follow before making the decision to dispense medicines or to refer to the physician. The four highlighted criteria in this study were: suspected ADR, duration of the health problem ≥7 days, medicines use currently for other health problems and pregnancy/lactation. Two of them are related to the medication, one of them with the HP or minor ailment and the other one with the patient.
In relation to the suspected ADR, the probability of referral to the physician and not to dispense medicines was approximately six times higher. This was expected, because the ADR can have a variable severity and can imply: death, life threatening, hospitalization, disability, congenital anomalies or defects32. According to these conditions, pharmacists decide not to dispense medicines. This justifies this criterion as part of the minor ailments service guidelines or protocols.
Contrarily, the duration of the health problem ≥7 days criterion is a less uncertain fact than the suspected ADR and is part of the basic knowledge that the community pharmacist must have. In much scientific literature about HP and its management, the duration of the health problem ≥7 days criterion is something already established and MAS clinical practice protocols and/or guidelines are not the exception.
Depending on the HP, excessive duration is usually the indicator to consider that it is not a minor ailment, so it requires more attention and a more detailed management by the corresponding health care professional1,5,14. In this study, the probability of referral to the physician and not dispense medicines according to the duration of the health problem ≥7 days criterion was approximately three times higher. This result may imply that the reason for the consultation could be a serious HP or its complication evolving slowly.
The probability of referral to the physician and not dispense medicines according to the criterion medicines use currently for other HP and the criterion other HP was approximately three times higher. These criteria suppose a greater complexity in the pharmacotherapy management of the patient according to pluripathology, polymedication, risk of drug-drug and drug-food interactions, as well as contraindications that must be assessed as part of the MAS and community pharmacist could refer to the physician or other pharmaceutical care services.
In the case of the pregnancy/lactation criterion, the probability that the pharmacist refers to the physician was three times higher. This result is not surprising because of the potential implications of the use of medicines in these conditions, for both the mother and the child. Pregnancy implies a certain number of physiological and biochemical modifications for the mother and fetus, which can affect the efficacy or tolerance of medications. As well as the risk of fetal toxicity, real or potential, which also has a relationship with the time of pregnancy16.
Finally, with the criterion medicines taken for the HP in question, the probability that the pharmacists should refer to the physician was approximately two times higher. According to that, it could be evidence of: a) that HP is not self-limiting or b) medicines have not been effective. Before the pharmacist refers to the physician he should evaluate: the correct administration of the medicines, the correct dose, the duration of the treatment and the medication schedule7.
As it was mentioned before, there is no regulation for the MAS in Costa Rica. This situation encourages the national debate and research in topics such as: the definition and classification of minor ailments, the definition of referral criteria with other healthcare professionals, the need for clinical guidelines or protocols, the documentation of outcomes11,29, and the medications list for this service3-5. In many countries, the elements associated with MAS are: different patient groups, service specifications (only patient advices, advices plus medicines from specific formulary, advices plus a referral to a more appropriate health professionals), the minor ailments (variety, complexity), the use of OTC or prescription medicines, pharmacists or appropriately trained staff members and forms of reimbursement23.
The main limitation of this study was that a representative sample of the community pharmacies was not included, but it shows part of the reality of the MAS in the country.
According to this study, the MAS in Costa Rica is complex and shows that the pharmacist follows a series of criteria to make a decision –the referral to physician or dispensing medicines–.
There are seven important criteria that Costa Rican pharmacists included in this study follow in the MAS. However, the one that stands out is Suspected ADR, followed by medicines used currently for other HP, duration of the HP ≥7 days and pregnancy/lactation.
Conflicts of interest: The authors declare no conflicts of interest.
BIBLIOGRAPHY
1. Good Pharmacy Practice Working Group from the General Pharmaceutical Council of Spain. Good Pharmacy Practice in Spanish Community Pharmacy: Minor Illness Service. Madrid, Spain. General Pharmaceutical Council of Spain. 2014.
2. Watson MC, Ferguson J, Barton GR, et al. A cohort study of influences, health outcomes and costs of patients’ health-seeking behaviour for minor ailments from primary and emergency care settings. BMJ Open 2015; 5:e006261. DOI:10.1136/bmjopen-2014-006261. Available at: https://bmjopen.bmj.com/ content/5/2/e006261.
3. Paudyal V, Watson MC, Sach T, et al. Are pharmacy-based minor ailment schemes a substitute for other service providers? A systematic review. Br J Gen Pract. 2013. DOI: 10.3399/bjgp13X669194. Available at: https://www.ncbi.nlm. nih.gov/pmc/articles/PMC3693804/pdf/bjgp-july2013-63-612-e472.pdf.
4. American Pharmacists Association. OTC Advisor Monograph 1. The Pharmacist’s Role in Self-Care [Internet]. American Pharmacists Association. Estados Unidos. 2009.
5. International Pharmaceutical Federation. FIP Statement of Policy – Pharmacy: Gateway to Care. The Hague: FIP, 2017. Available at: www.fip.org/statements.
6. Salar L, Prats R, Eyaralar T, Espejo J. Programa ‘I-Valor’: la indicación farmacéutica protocolizada, consensuada y registrada en la farmacia comunitaria. Farmacéuticos Comunitarios. 2017 Sep 30;9(3):5-12. DOI:10.5672/ FC.2173-9218.(2017/Vol9).003.02.
7. Foro de Atenció́n Farmacéutica Farmacia Comunitaria. Guía Práctica para los Servicios de Atenció́n Farmacéutica en la Farmacia Comunitaria. Madrid, España: Consejo General de Colegios Oficiales de Farmacéuticos; 2010. Available at: https://www.portalfarma.com/inicio/serviciosprofesionales//forofarmaciacomunitaria/Documents/ATFC_Guia%20FORO.pdf.
8. Pereira A, Lizano C, Hernández LE. Caracterización de las consultas de Indicación Farmacéutica en 30 farmacias comunitarias del área metropolitana de Costa Rica. Pharm Care Esp. 2016;18(1):16-27.
9. Lizano C. Protocolos de Indicación Farmacéutica en síntomas menores gastrointestinales para farmacias de comunidad de Costa Rica (Primera parte). Pharm Care Farmacoter. 2014;1(1):1-25.
10. Jimenez A, Rojas T, Arias F. Caracterización de los servicios brindados en las farmacias de comunidad privadas de Costa Rica. Pharm Care Farmacoter. 2012;1(1):4-10.
11. Prats R, Roig I, Baena MI, García-Delgado P, Martínez-Martínez F, Amariles P. Actuaciones profesionales realizadas en la farmacia comunitaria. Pharm Care Esp. 2012;14(5):193-201.
12. Pastor R, Alberola C, Álvarez de Toledo F, Fernández de Cano N, Solá N. Clasificación de Derivaciones Fármaco-Terapéuticas. Madrid, España: International Marketing & Comunnication S.A. (IM&C); 2008.
13. Llanes de Torres R, Aragón A, Sillero MI, Martín MD. ¿Ir al centro de salud o bajar a la farmacia? Las oficinas de farmacia como recurso de atención primaria. Aten Primaria. 2000;26(1):11-15.
14. Machuca M, Baena M, Faus M. Programa IndDáder. Guía de Indicación Farmacéutica. Granada, España: Grupo de investigación en Atención Farmacéutica Universidad de Granada. 2005. p 33.
15. World Health Organization. Health Impact Assessment (HIA): The determinants of health [Internet]. 2020. Available at: https://www.who.int/hia/evidence/doh/en/.
16. Belon JP. Consejos en la farmacia. Editorial Masson. S.A. Barcelona, España. 1995.
17. Consejo General de Colegios Oficiales de Farmacé́uticos. Foro de Atención Farmacéutica (FORO). Madrid, España: 2008. Available at: https://www.portalfarma.com/inicio/serviciosprofesionales/forodeattfarma/Documents/FORO_At_farma.pdf.
18. Ministerio Sanidad y Consumo de España. Consenso sobre Atención Farmacéutica [Internet]. Madrid, España. 2001. Available at: http://www.sefh.es/ consenso/consenso.pdf.
19. Machuca M, Machuca MP, Gastelurrutia P, Gutiérrez Aranda L, Fernández López E, Romero Barba L. La indicación farmacéutica disminuye las visitas al médico y resuelve las demandas de los pacientes. Seguim Farmacoter. 2003;1(3):110-4.
20. Raferty E, Yaghoubi M, Taylor J, Farag M. Costs and savings associated with a pharmacists prescribing for minor ailments program in Saskatchewan. Resour Alloc. 2017;15:3. DOI: 10.1186/s12962-017-0066-7.
21. Guirguis LM, Hughes CA, Makowsky MJ, et al. Development and validation of a survey instrument to measure factors that influence pharmacist adoption of prescribing in Alberta, Canada. Pharm Pract. 2018. Jan-Mar;16(1):1068.
22. Mansella K, Bootsmana N, Kuntzb A, Taylora J. Evaluating pharmacist prescribing for minor ailments. International J Pharm Pract. 2015;23: 95-101. DOI: 10.1111/ijpp.12128.
23. Aly M, García-Cárdenas V, Williams K, Benrimoj SI. A review of international pharmacy-based minor ailment services and proposed service design model. Res Social Adm Pharm. 2018;14(11):989-998. Published 2018 Jan5. doi:10. 1016/j.sapharm.2017.12.004.
24. Habicht D, Ng S; Dunford D, Shearer B, Kuo I. Incorporating assessment and prescribing for ambulatory ailments skills into practice: An environmental scan of continuing education for pharmacist prescribing in Canada. Can Pharm J. 2017 Jul 31;150(5):316-325. DOI: 10.1177/1715163517723352.
25. Dineen-Griffin S, Garcia-Cardenas V, Rogers K, Williams K, Benrimoj SI. Evaluation of a Collaborative Protocolized Approach by Community Pharmacists and General Medical Practitioners for an Australian Minor Ailments Scheme: Protocol for a Cluster Randomized Controlled Trial. JMIR Res Protoc. 2019;8(8): e13973. Published 2019 Aug 9. doi:10.2196/13973.
26. Eikenhorst L, Salema N, Anderson C. A systematic review in select countries of the role of the pharmacist in consultations and sales of non-prescription medicines in community pharmacy. 13(2017)17-38. Res Soc Adm Pharm. 13(2017)17-38. Available at: https://doi.org/10.1016/j.sapharm.2016. 02.010.
27. González D, Acuña A, Castillo A, Fornos JA, Andrés JC, Andrés NF. Implementación de procedimientos de indicación y dispensación en farmacias comunitarias de la provincia de Pontevedra tras una acción formativa. Técnica del paciente simulado. Pharm Care Esp. 2011;13(3):104-113.
28. Inch J, Porteous T, Maskrey V, et al. It’s not what you do it’s the way that it’s measured: quality assessment of minor ailment management in community pharmacies. Int J Pharm Pract. 2017.25:253-262. Available at: https://doi.org/ 10.1111/ijpp.12305.
29. Egorova SN, Akhmetova T. Pharmaceutical counseling: Between evidence based medicine and profits. Int J Risk Saf Med. 2015.27(1):S878. DOI: 10.3233/ JRS150701.
30. World Health Organization. Noncommunicable diseases country profiles 2018 [Internet]. 2018. Available at: https://www.who.int/nmh/publications/ncd- profiles-2018/en/.
31. Sáenz M, Acosta M, Muiser J, Bermúdez JL. Sistema de salud de Costa Rica. Salud pública Méx. 2011.53(2):s156-s167. Available at: http://www.scielo.org. mx/scielo.php?script=sci_arttext&pid=S0036-36342011000800011&lng=.
32. Papale R, Schiaffino S, García MG. Manual de Buenas Prácticas de Farmacovigilancia Edición Lationamerica. 1 ed. Ciudad Autónoma de Buenos Aires. Ediciones Farmacológicas 2018.
____
